I asked my doctor for an Omega-3 index three years ago. He rejected it. He claimed there wasn’t any evidence for managing Omega-3 levels. It also wasn’t covered by my health insurance. And I left my appointment disappointed by the reasoning. Now, three years later, many more studies have been published. What exactly are Omega-3s? Should you get a test to measure it? And what guidelines should you follow to achieve optimal results? Well, let’s get into it!
What are Omega-3 Fatty Acids?
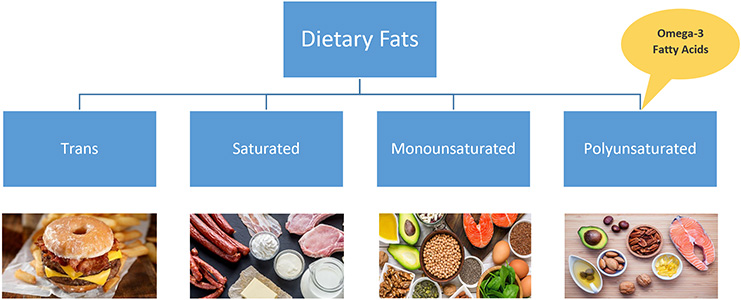
Dietary fats fall into four categories: Trans-fat which is banned in the United States [1]. Saturated fat which is villainized in the United States [2]. Monounsaturated fat and Polyunsaturated fat which are generally recommended based upon the source. Omega-3 fatty acids fall into the fourth, polyunsaturated fat category. Humans can’t produce these Omege-3 fatty acids and require intake from dietary sources [3].
I remember in the early 2000’s, my dad placed special importance on consuming these Omega-3 polyunsaturated fats. He’d have salmon weekly at dinner. And he’d swallow these large yellow fish oil pills. It turns out, this resulted from a landmark Omega-3 study published in 1999. It found that supplementing 1 g/day of Omega-3 resulted in a significantly lower risk of death [4]. This research led many, like my dad, to make Omega-3 the most popular nonvitamin/nonmineral supplement by 2012 [5]. But research over the past 20 years is starting to uncover more nuance.
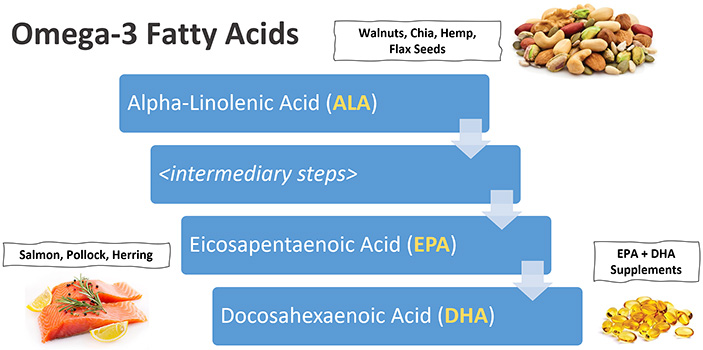
α-Linolenic acid (ALA) is a type of Omega-3 found in plants and algae. Specifically, walnuts, chia seeds, hemp seeds, and flax seeds. Then there’s Eicosapentaenoic Acid (EPA) and Docosahexaenoic Acid (DHA). ALA can be converted into EPA and DHA, but this process may be insufficient in humans. Only 10–14% of ALA eventually becomes EPA and DHA. If you were to only consume ALAs, you’d risk being low in EPA and DHA. But these types can be found in fatty fish like salmon, pollock, and herring. Or, with supplementation. Now the reason fatty fish have EPA and DHA is because they frequently consume algae or other algae eating fish. Algae is rich in ALA and fish convert that to EPA and DHA efficiently. It’s why our Omega-3 levels are most affected by our fish consumption. But does consuming these Omega-3 fatty acids provide any substantial benefits? [7]
Why Should We Measure it?
Shortly after the landmark 1999 study, others like the OMEGA study found no benefits from the 1 g/day supplementation. No decreased risk of death. No depressed cardiovascular risk. Further controversy found Omega-3 supplements increased prostate cancer risk. These studies questioned the use of Omega-3 supplements altogether. Ultimately, a more thorough review found the prostate claims to be false. [4]
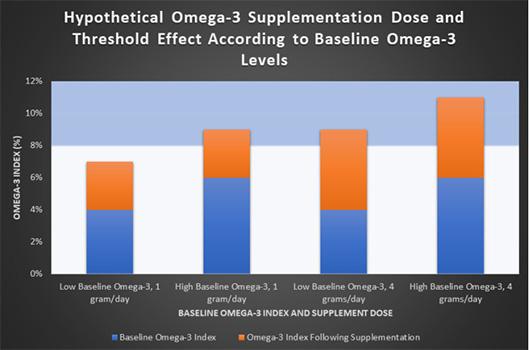
Regarding heart disease, humans may need to meet a certain threshold of Omega-3 to receive therapeutic benefits. The landmark 1999 study, and others like it, had populations with high Omega-3 levels already. From a fish rich diet. And the 1 g/day of Omega-3 supplements, put them over the therapeutic threshold. They saw heart health benefits. But the opposing studies had populations with low Omega-3 levels. Therefore, the 1 g/day of Omega-3 didn’t appear to be enough to reach the therapeutic threshold. They didn’t see any benefit because they didn’t consume enough. But this is just a theory. Studies have shown conflicting results with heart disease. [4]
A bigger effect may be seen with the brain. 50-60% of the brain is made of fat. 35% of that fat is Omega-3. All that Omega-3 improves blood circulation in the brain. This promotes cognition, neuronal preservation, and protection against neurodegeneration [7]. Meaning you’ll stay sharper for longer. You’ll be more likely to ward off Alzheimer’s and dementia with age. Omega-3 may help with depression, loneliness, learning, and memory too. While I think more research is needed to confirm the effects and magnitude of effects, optimizing Omega-3 levels may be worthwhile. But how can you test your levels and what’s the ideal result?
How to Measure it? Ideal Results?
An Omega-3 Index is a blood test of EPA and DHA levels. While many health insurance companies may not cover it yet, you can buy an online test for under $100. My brother and sister did just that. I went to Quest labs in January to test numerous metrics. Unfortunately, 90% of my tests failed to make it to the correct lab due to a snowstorm… Somehow, my Omega-3 index was fortunate enough to make it. My index tested at 1.1% EPA and 2.8% DHA. Totaling 3.9% overall. Lower than I would have liked. This may be due to my lack of supplementing all of December… because Vicki may or may not have lost my mailbox key… which had my latest shipment of supplements in them. I’m hoping to test again soon for a more accurate result.
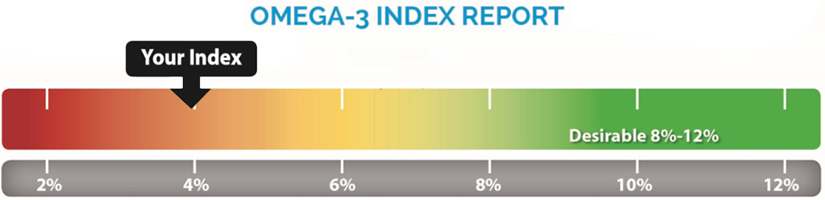
But an Omega-3 index below 4% has been proposed as an indicator of increased health risk. This is also the average American serum level. Meaning the average American is low and at risk. This is because Americans eat few fish and fish is the primary determinant of Omega-3 levels. But to be in the lowest-risk category, studies suggest being above 8% [4]. I am cautious of this number though.
First, it’s hard to reach 8% without large doses of supplements or binging on fatty fish. Neither of which may be beneficial. Second, most of the studies are associations and not cause and effect. Fish consumption may improve the average Americans diet resulting in the positive benefits while the Omega-3 index may just be an associated metric. A metric that could be artificially inflated by Omega-3 supplements. Third, running cause and effect, randomized controlled trials, take a long time to tease out cognitive decline. While there aren’t many to date, a 3-year study using Omega-3 supplements as an intervention showed no positive effects. This could mean positive effects are only seen decades after consistent consumption. An effect that may be hard to prove. [8]
So, I’m not fully convinced we all need to aim for 8% as I’m not fully convinced of the benefits. But I don’t want to be below 5%. I guess I’m hedging my bets for now until more research is published. Especially since Omega-3 supplements are well-tolerated, low risk, and potentially beneficial [7].
Protocol to Manage it
Either way, if you want to go for 8% or avoid being below 5% like me, here’s how to accomplish it. Fatty fish are the primary source. The current dietary guidelines for Americans recommend consumption of approximately 8 ounces per week. That’s equivalent to two medium servings. Fatty fish like salmon, pollock, and herring would be expected to provide an average daily intake of approximately 250 mg of EPA and DHA. However, that amount will not increase your Omega-3 index to a level > 8%. Therefore, it’d require a supplement of 1 to 2 g/day of EPA + DHA. [4]
If you’re avoiding fish and want to reach that 8% target, you’d need a higher dose supplement around 2-4g/day of EPA + DHA. Why might you avoid fish? Their frequent consumption exposes us to mercury, which is especially harmful [6]. The consumption of pork, eggs, fish, and other seafood accounts for over 90% of toxic PCB consumption too [9]. This is because our ocean waters are polluted. So, while the benefits of 8oz of fish a week outweigh these risks, I personally avoid seafood. And I’d recommend limiting it to the 8oz a week recommendation while selecting low-mercury, wild caught, high Omega-3 fish.
Instead, I opt for one serving a day of walnuts, hemp, chia, and flax seeds. That’s four total servings a day of high ALA foods. This helps mediate our inefficient ability to convert ALA to EPA and DHA. And then I take an algae-based Omega-3 supplement containing 200mg of EPA and 400mg of DHA. While I’m only a N of 1, and I need to retest for confirmation, I think this combination should take me to my current Omega-3 index goal of 5%. But if more research prevails, I’m open to reframing my protocol and goal. I want to do whatever proves optimal.
Final Thoughts
Omega-3 fatty acids are a type of polyunsaturated fat. They must be consumed from food because humans can’t manufacture it. And since most Americans don’t consume fish, and fish is our primary vehicle for Omega-3, most Americans are low in Omega-3. This may have detrimental effects on our cardiovascular and nervous systems. Potentially, increasing our risk for cognitive decline and dementia with age. But this isn’t confirmed by all studies. While studies recommend Omega-3 levels above 8% to be in the lowest risk category, I’m taking a more cautious approach of 5%. I’m planning to test my levels every few years and adjust my goal and supplement upon future scientific research. But for now, these are my latest habits for health excellence.

